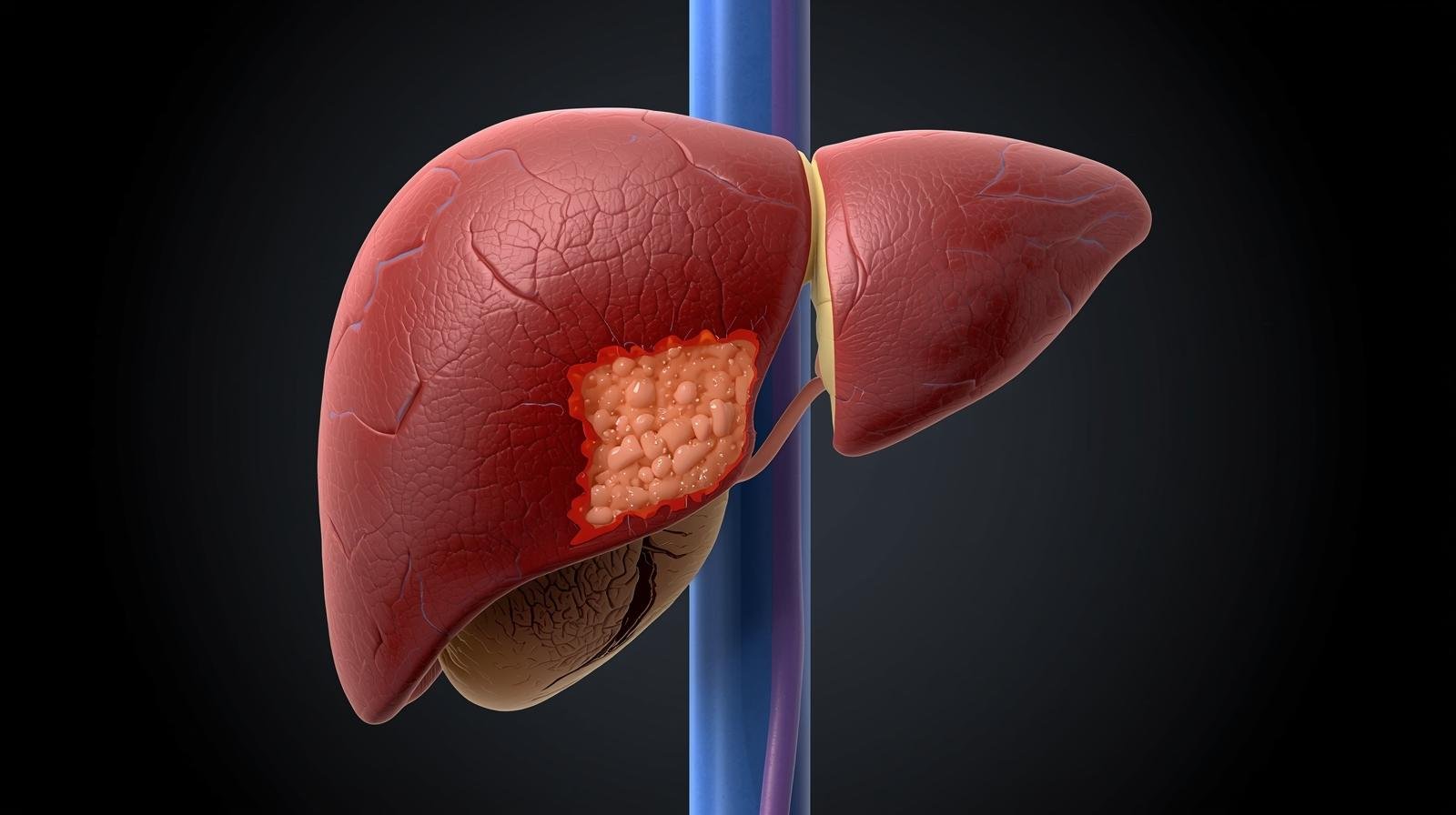
Silent fatty liver disease refers to a condition where excess fat accumulates in the liver without obvious symptoms. Traditionally called Non-Alcoholic Fatty Liver Disease (NAFLD), it has recently been renamed Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) to better reflect the underlying metabolic causes like obesity, diabetes, and high cholesterol — not alcohol use.
In most people, this fat buildup doesn’t cause pain or clear early symptoms, so many are unaware they have it. Most cases begin as simple steatosis (fat without liver cell injury) and may remain stable. However, without detection and management, it can progress to more severe disease.
Why “Silent” Doesn’t Mean “Harmless”?
Even without symptoms, silent fatty liver can progress to inflammation and scarring. When fat in the liver triggers inflammation and liver cell damage, the condition is termed non-alcoholic steatohepatitis (NASH) or in newer terminology, metabolic dysfunction-associated steatohepatitis (MASH).
This inflammation can lead to fibrosis (scar tissue), and over time, advanced scarring may progress to cirrhosis — a late stage of liver disease in which normal liver structure is replaced by scar tissue. Severe cirrhosis can ultimately lead to liver failure, where the liver can no longer function properly.
How Common and Serious Is It?
Silent fatty liver disease is very common worldwide, especially among people who are overweight, have type 2 diabetes, high blood pressure, or abnormal cholesterol levels. Many individuals may never progress to advanced disease; but for a subset, progression is real and serious.
In clinical studies, about 20% of those with NASH go on to develop significant liver disease, including cirrhosis and liver-related complications. Even then, progression may take years or decades, and early stages often lack symptoms.
Common Causes and Risk Factors
Silent fatty liver develops when excess fat is stored in liver cells, usually due to metabolic dysfunction. Major risk factors include:
- Overweight and obesity
- Type 2 diabetes or prediabetes
- High triglycerides or abnormal cholesterol
- High blood pressure
- Metabolic syndrome
Because these risk factors are common, especially with sedentary lifestyles and calorie-rich diets, silent fatty liver has become a major public health issue.
Why It Often Has No Early Symptoms?
The liver has remarkable capacity to function even when stressed. Early in the disease, many people have normal liver blood tests and no complaints. Even minor elevations in liver enzymes don’t reliably predict how advanced the disease is.
Some people may notice vague signs such as fatigue, mild discomfort in the upper right abdomen, or weakness — but these symptoms are nonspecific and can easily be attributed to other causes.
How Doctors Detect Silent Fatty Liver?
Because symptoms are subtle or absent, detection usually occurs through screening tests when risk factors exist:
- Lifestyle and medical history review
- Blood tests: Liver enzymes, glucose, lipids
- Fibrosis risk scoring (e.g., FIB-4, NAFLD fibrosis score) to estimate scar risk
- Imaging tests like ultrasound, FibroScan, or MRI to evaluate liver fat and stiffness
General population screening (testing everyone without risk factors) is not recommended. Targeted assessment in people with metabolic risk factors helps identify those at highest risk.
Treatment: What Works and Why?
There is no single “magic pill” for silent fatty liver — lifestyle changes are the cornerstone of care:
Lifestyle Interventions
Weight loss: Reducing 5%–10% of body weight can significantly reduce liver fat and inflammation.
Diet: A hypocaloric diet that emphasizes whole foods (like the Mediterranean diet) can reduce fat accumulation and improve metabolism.
Exercise: Regular physical activity improves insulin sensitivity and helps reduce liver fat.
Medications
Currently, specific medications are generally reserved for those with confirmed NASH and significant fibrosis, not for everyone with simple silent fatty liver.
Other Therapies
In selected individuals with severe obesity and metabolic dysfunction, bariatric surgery may be considered and has shown benefit in reducing liver fat and improving histological features of NASH.
Preventing Progression: Practical Steps
To prevent silent fatty liver from advancing:
- Maintain a healthy weight through diet and exercise
- Control diabetes and metabolic risk factors
- Limit alcohol intake
- Avoid smoking
- Regular check-ups if you have risk factors like obesity or diabetes
- Work closely with healthcare providers to monitor liver health
Lifestyle changes not only help the liver but also reduce the risk of heart disease, stroke, and type 2 diabetes, all of which are linked to metabolic dysfunction.
Conclusion
Silent fatty liver disease is common, often symptomless, and can progress over time toward inflammation, fibrosis, cirrhosis, and ultimately liver failure if unrecognized and untreated. The key message for the general population is that early detection and lifestyle change matter, even if you “feel fine.” Regular check-ups in the presence of risk factors and sustained healthy habits can halt or sometimes reverse the disease.
Sources
- AASLD Practice Guidance on NAFLD clinical assessment and management – PubMed PMC. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10735173/
- EASL-EASD-EASO Clinical Practice Guidelines for NAFLD – Obesity Facts (Karger). https://karger.com/ofa/article/9/2/65/241098
- Italian Clinical Practice Guideline on NAFLD – PubMed. https://pubmed.ncbi.nlm.nih.gov/34914079/
- NAFLD diagnosis and management (AAFP). https://www.aafp.org/pubs/afp/issues/2023/0500/practice-guidelines-nonalcoholic-fatty-liver-disease.html
- Non-alcoholic fatty liver disease patient guideline – PubMed PMC. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8514420/
- Cleveland Clinic overview on NAFLD management. https://my.clevelandclinic.org/departments/digestive/medical-professionals/hepatology/nonalcoholic-fatty-liver-disease
- Verywell Health: What’s New in MASH Treatment?. https://www.verywellhealth.com/what-s-new-in-mash-11708862